
Getting students up to speed in clinic is a common challenge due to the fast pace of the clinical environment, the amount of content to learn, limited faculty time, and the lack of universal experiences.
Below, we’ll highlight three examples of how educators are using Aquifer to improve key clinical skills by:
- Using Aquifer to Meet Accreditation Standards for Targeted Remediation
- Pace University College of Health Professions Physician Assistant Program
- Covering Geriatrics Across the Curriculum
- Mayo Clinic Alix School of Medicine
- Using Aquifer for the Focused Physical Exam
- University of Colorado Child Health Associate/Physician Assistant Program
Using Aquifer to Meet Accreditation Standards for Targeted Remediation
At the Pace University College of Health Professions Physician Assistant program, in addition to using Aquifer for flipped classroom sessions, assessing written documentation such as SOAP notes, and evaluating oral presentation skills in the clinical year, faculty at Pace also use Aquifer for targeted remediation.
Using Aquifer for individualized clinical exam remediation not only addresses gaps in students’ clinical reasoning but also helps meet ARC-PA standard B4.01, which requires programs to conduct frequent, objective, and documented evaluations of student performance and then identify and address any student deficiencies in a timely manner.
Because of the very hectic schedules for students during the clinical year and the fact that students take different rotations at different times, it is essential to identify knowledge gaps as quickly as possible and remediate them. Pace uses PAEA End of Rotation exams that give feedback by keyword. Using this feedback, faculty use the Aquifer content library to quickly find patient cases that help address these gaps and assign them to students. Students do the cases on their own schedule and then re-test, if necessary, the following week.
“I cannot express how useful Aquifer has been in enhancing and strengthening our assessment tools during the fast-paced clinical year.”
– Shannon North, MS, PA-C
Remediating clinical reasoning errors
Pace faculty also use Aquifer to remediate clinical reasoning, helping students reflect on their own cognitive errors and biases. Faculty noticed in their simulated case lab that students were immediately diagnosing a standardized patient case with a previous medical history of asthma who presents with acute shortness of breath with acute asthma exacerbation without considering other differential diagnoses.
To remediate this clinical reasoning deficiency, typically, the program would have to reschedule lab time, which could take months. Rescheduling burdens both faculty and students in terms of resources and time available and does not provide remediation in a timely manner.
By assigning a specific Aquifer case with a similar scenario (Aquifer Diagnostic Excellence Mini-Case 05A: Internal Medicine), they were able to close this learning gap. Faculty had students complete the case, watch the video of the standardized patient encounter, and write a guided reflection on their own cognitive biases and errors.
Covering Geriatrics Across the Curriculum
At the Mayo Clinic Alix School of Medicine (MCASOM), faculty were concerned that their geriatrics curriculum was weak due to the lack of a mandatory geriatrics clerkship. To meet their goals of teaching the national geriatrics competencies (the “5 Ms”) without adding a dedicated geriatrics clerkship, they turned to Aquifer to help cover the necessary objectives. Because Aquifer Geriatrics is tied to these core competencies, the cases were able to help bridge this gap.
As a school, MCASOM developed a system that integrated Aquifer Geriatrics cases in all of their required clerkships (other than pediatrics). Each of the cases that were used directly related to the learning occurring within the clerkship. Using the chart below, which is found in the Aquifer Geriatrics Educator Guide, they were easily able to find geriatrics cases linked to their clerkships.
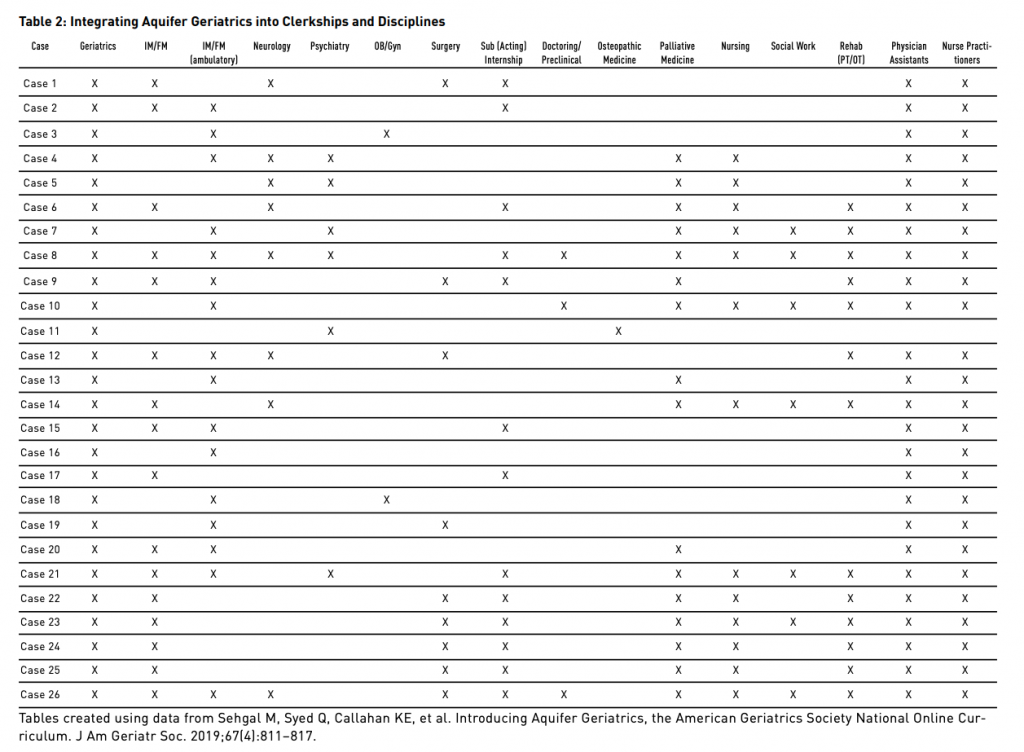
For example, in students’ OB-GYN clerkship, MCASOM uses Aquifer Geriatrics cases 03 and 18 to cover urinary incontinence and the aging physiology of the bladder, two of the national competencies. These cases are first completed by students outside of clinic. Then, students learn appropriate methods for performing a pelvic exam on an aging person and build an understanding of the types of incontinence working in clinic with their preceptor.
Over the course of their clinical years, students will complete 16 different Aquifer geriatrics cases integrated across all required clerkships (excluding Pediatrics), as well as their Emergency Medicine clerkship and 4th-year Sub-I, covering all of the core competencies along the way.
“Aquifer has enabled us to create a geriatrics-infused clinical curriculum without any extra curricular time”
– Amit Shah, MD, FACP, AGSF
Faculty report that students have been very receptive to being assigned the cases because of the intentionality of the way they are assigned and how they are directly tied to their clerkships. Furthermore, because MCASOM has campuses in three states in three different time zones, using Aquifer cases link allows for easy tracking of student progress and standardization of experience between locations.
Using Aquifer for the Focused Physical Exam
At the University of Colorado Child Health Associate/Physician Assistant Program (CHA/PA), faculty are using Aquifer cases to hone their clinical reasoning skills and reinforce medical knowledge with 2nd and 3rd-year students. During these clinical years, students have a weekly clinical medicine case time where they are given an hour to review an Aquifer case and then a debrief with a content expert.
During their musculoskeletal unit in their second year, one of these debriefing sessions is centered on Aquifer Family Medicine 11. In this case, a patient presents at the clinic with knee pain and later returns with wrist pain. During the debriefing section, faculty have students practice the focused physical exam of the wrist on their classmates in pairs, given this chief complaint. Faculty walk around and observe students practicing the physical exam of the wrist on each other, followed by a discussion led by the facilitator focused on the physical exam. During the debriefing session, the facilitator leads a discussion, asking pointed questions such as:
- How did the learner decide which exam elements needed to be performed?
- How did each exam element and finding either support or refute the learner’s hypothesis on the differential diagnosis?
- Were there specific special tests performed and why?
Students have previously learned in their first year how to perform this specific exam, so it also provides a good opportunity to revisit and reinforce that topic during their second year.
Both students and faculty at CHA/PA like the cases because they are robust. Faculty have found that the Aquifer cases are ideal for intermediate and advanced learners because they can typically go through the cases at their own pace without the need for faculty assistance. The standardization of the debrief is helpful for students, and it also allows outside content experts to come in more easily and be able to get up to speed quickly.
To hear more about the details of these debriefing sessions, please listen to our podcast with Kelsey Dougherty, MMSc, PA-C, and download the template to follow along as she and host Lynne Robins walk through the template.
Learn More
Watch our on-demand webinar, Strategies for Teaching Clinical Skills with Aquifer, where you’ll get even more details on these examples and others from faculty across the country who are putting Aquifer to work for their students.




