By: Sherilyn Smith, MD | Clinical Skills Learning Specialist | University of Washington | Aquifer Chief Academic Officer
The pandemic caused by SARS-CoV-2 (COVID-19) created widespread disruption for healthcare professional education throughout the world. Healthcare professional students were rapidly removed from clinical settings and schools swiftly modified instruction and restructured curricula.
At Aquifer, we saw an unprecedented jump in the use of our virtual patient cases as medical schools and health professions programs took advantage of our free access offer and discovered innovative new ways to implement cases across their curricula. Through our grant applications and ongoing conversations with educators, we were able to identify trends and challenges and share innovative and successful use cases.
Identifying Trends & Challenges
In May 2020, Aquifer surveyed programs using our cases–as part of the application process for Full Course Library Grants–about their current challenges, instructional methods for the next 6 months, and use of Aquifer cases. A total of 198 programs responded to the survey, including U.S. medical schools, osteopathic medical schools, physician assistant programs, and a few nurse practitioner programs.
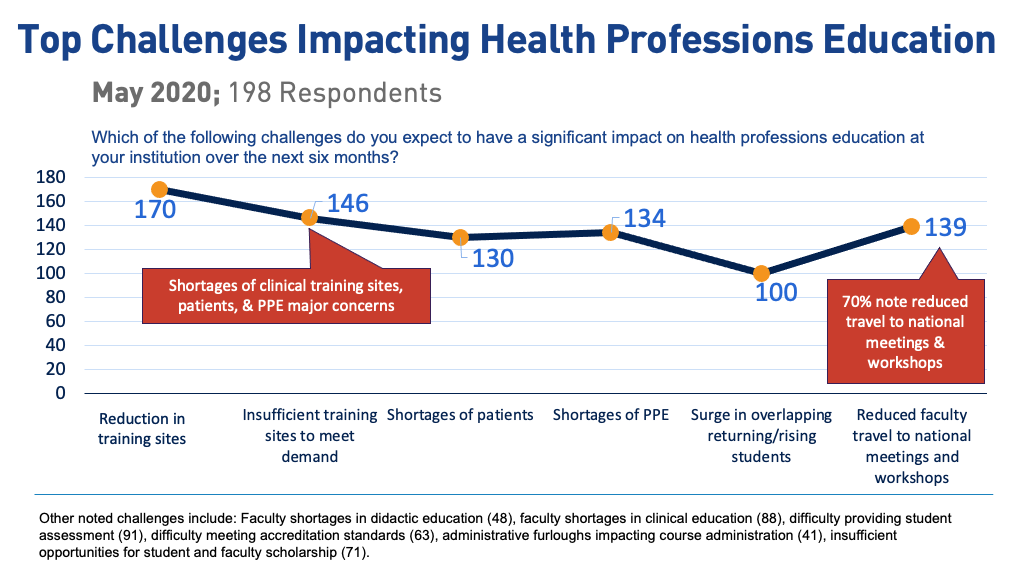
Survey respondents overwhelmingly responded that they were planning for hybrid instruction for the remainder of 2020 for both clinical (87%) and pre-clinical/didactic (80%) learning, as opposed to all in-person or all virtual instruction. We also noted that 70% of programs selected reduced travel to national meetings and workshops as a significant challenge, highlighting an ongoing need for faculty development and collaboration in our increasingly virtual world.
The most widespread challenge impacting health professions education–noted by 90% of survey respondents–was the reduction in training sites, with 77% expecting that training site availability would be insufficient to meet the needs of their educational programs. Additional factors compounding the difficulty in providing clinical education for responding programs included lack of sufficient PPE for students, faculty being deployed to care for patients and not being available for teaching, and an insufficient number of patients in clinical settings.
Successful Strategies & Innovative Integration
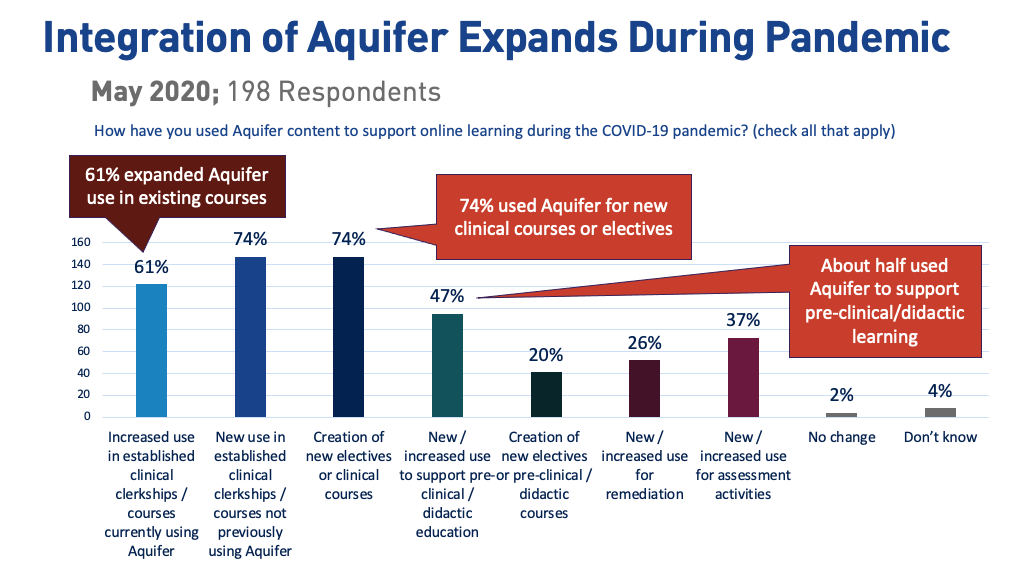
Educators were highly creative during the pandemic with their use of Aquifer cases. Early in the pandemic, programs reported expanding their use of Aquifer in existing clinical phase courses, creating new courses and electives using Aquifer cases, adding Aquifer cases to pre-clinical/didactic phase courses, expanding their use of Aquifer for assessment, and using Aquifer for remediation.
As Aquifer endeavored to support faculty development and community this year, many talented educators shared their successful strategies with their colleagues through our webinars and blogs. We have seen some very interesting and innovative ways that faculty have integrated Aquifer cases into their curricula this year. Here are just a few of our favorites:
- Building Clinical Communication Skills
In the absence of live patients, a number of schools have used Aquifer cases to enhance students’ clinical skills by assigning cases and having students write SOAP notes and/or do oral case presentations to their peers. - Efficient Preparation to Optimize Limited In-person Learning
Faculty facing shorter clinical rotations have used Aquifer cases to build remote rotations on core conditions, completed prior to seeing real patients. Programs have also designed orientation courses for the transition to clinical years and hospital systems to deliver key content online and make the most of limited in-person instruction time. - Framework for Discussions & Engaging Didactics
With Aquifer cases as pre-work, faculty engaged students online in small group discussions, working through compare and contrast exercises, and using our own active learning teaching tools (Pediatrics Case Analysis Tool, Radiology Flipped Classroom Workshops). - Bringing Basic Science to Life
Our colleagues have reported using Aquifer cases in basic science classes to reinforce key practical concepts about pharmacology and mechanisms of action, thus bridging basic and clinical sciences. - Journal Club
Some of our physician assistant colleagues have leveraged the evidence and articles embedded in each case to create journal clubs for their students. - Creating Virtual Courses & Electives on Special Topics
Educators are creating courses highlighting high value care, diagnostic reasoning, and using very engaging formats. We’ve even seen students work to design courses like this one on Tough Conversations and End of Life Care with virtual content.
Planning for the Future
As we enter winter of 2020-21 in the face of a pandemic surge, there remains significant uncertainty about the impact of COVID-19 on healthcare professions education. Educators are continuing to flex, with more programs allowing students to care for COVID-19 patients and expanded telemedicine options as a way to reach our patients and teach our students. As Dr. Skylar outlines in his commentary in Academic Medicine1 we have the opportunity to reshape how we provide high-quality healthcare education. Educators are innovating around the country and we anticipate that we will see a flurry of new methods that result in high-quality outcomes2-5.
We look forward to discussing strategies for overcoming and adapting to the challenges we’re facing in education and sharing more stories and successful innovations in our panel discussion at our upcoming webinar: Lessons Learned from COVID-19: Best Practices for Using Aquifer in Virtual Rotations.
At Aquifer, we will continue to share your innovations with our educational community and strive to help educators stay ahead of the curve, provide the support and education our students need, and provide faculty with resources to thrive in the coming year.
1. Lessons From the Disaster That Can Improve Health Professions Education. Acad Med. 2020 Nov;95(11):1631-1633. doi: 10.1097/ACM.0000000000003547. PMID: 32544103; PMCID: PMC7309647.
2. Iancu AM, Kemp MT, Alam HB. Unmuting Medical Students’ Education: Utilizing Telemedicine During the COVID-19 Pandemic and Beyond. J Med Internet Res. 2020 Jul 20;22(7):e19667. doi: 10.2196/19667. PMID: 32614776; PMCID: PMC740003
3. Hall AK, Nousiainen MT, Campisi P, Dagnone JD, Frank JR, Kroeker KI, Brzezina S, Purdy E, Oswald A. Training disrupted: Practical tips for supporting competency-based medical education during the COVID-19 pandemic. Med Teach. 2020 Jul;42(7):756-761. doi: 10.1080/0142159X.2020.1766669. Epub 2020 May 25. PMID: 32450049.
4. Lessing JN, Anderson LR, Mark NM, Maggio LA, Durning SJ. Academics in Absentia: An Opportunity to Rethink Conferences in the Age of Coronavirus Cancellations. Acad Med. 2020 Aug 25. doi: 10.1097/ACM.0000000000003680. Epub ahead of print. PMID: 32852317.
5. DeWitt DE. Fighting COVID-19: Enabling Graduating Students to Start Internship Early at Their Own Medical School. Ann Intern Med. 2020 Jul 21;173(2):143-144. doi: 10.7326/M20-1262. Epub 2020 Apr 7. PMID: 32259191; PMCID: PMC7151353.